With CIVHC’s Community Dashboard, users can identify how performance in critical health measures varies across Colorado communities and where the most significant opportunities lie for improvement and impact. Providers, payers, consumers, and other stakeholders can examine several aspects of care including cost, use of preventative services, utilization and access to care, and more.
Examining performance in each of these critical measures of care builds the framework to assess the health of communities across Colorado. In this data dive, we examine what the Community Dashboard reveals about pediatric care in Colorado, a crucial element of public health that is new to the most recent dashboard.
Measuring Pediatric Care
Three pediatric measures are now available to provide information on access to care for children and adolescents:
- Well-Child Visits First 15 Months, Six or More Visits
- Well-Child Visits 16 to 30 Months, Two or More Visits
- Well-Care Visits for Children and Adolescents
Well-child and well-care visits (for children 12 months to 19 years old) are essential to provide care information to parents or guardians and give comprehensive care for the child, including ensuring the child is up to date on immunizations and meeting growth and development milestones.
It is important to note that these measures only include children with commercial or Medicaid insurance. To learn more about these measures and others used in the dashboard, see the Community Dashboard Methodology.
Care Is Improving Across Colorado
CO APCD data from 2013-2020 shows that there is measured improvement across all pediatric measures in the Community Dashboard. Well-child visits for children in their first 15 months improved significantly, rising by 23% overall in that time, while visits for children between the ages of 16 and 30 months also ticked upward by 5% overall.
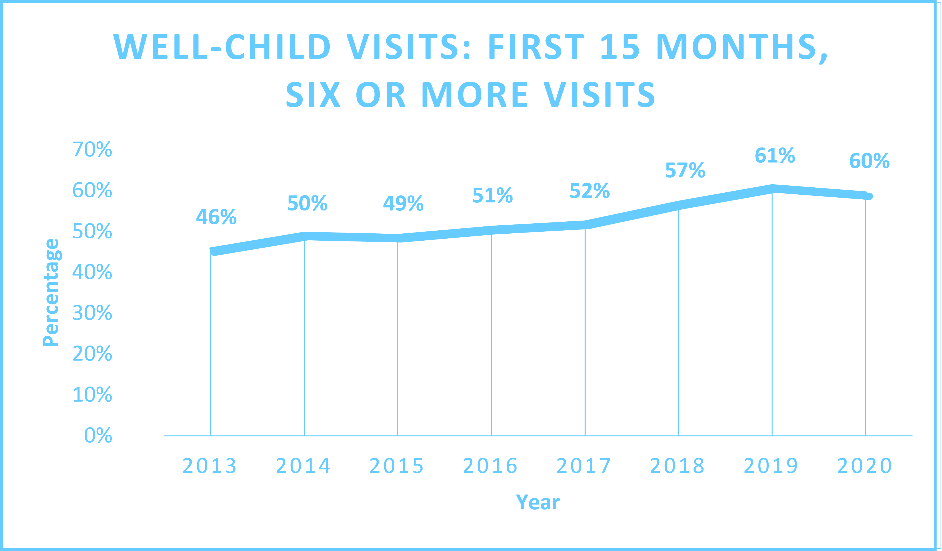
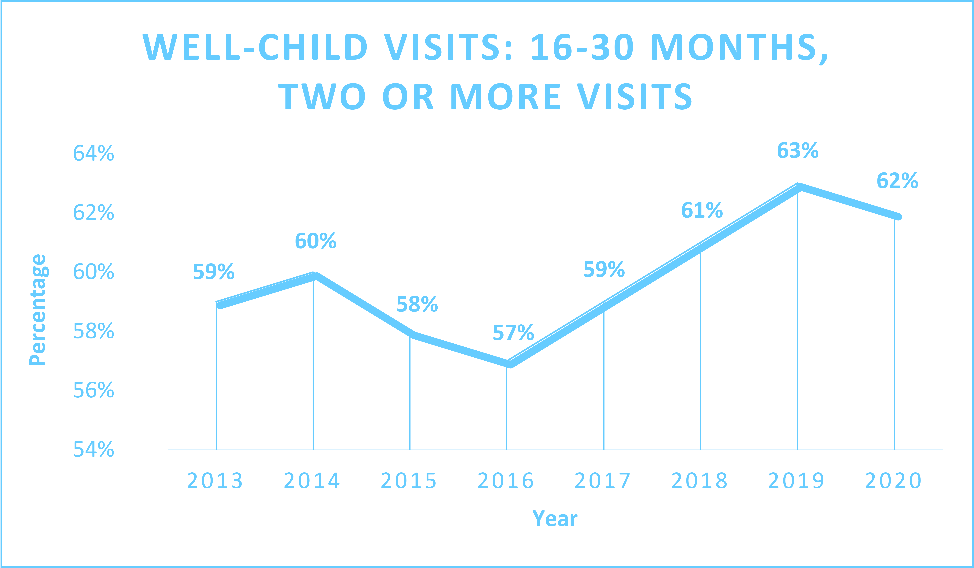
Meanwhile, the percentage of children and adolescents receiving annual well-care checks gradually improved since 2013, but did see a significant drop in 2020, likely due to the COVID-19 pandemic and decreased use of services overall.
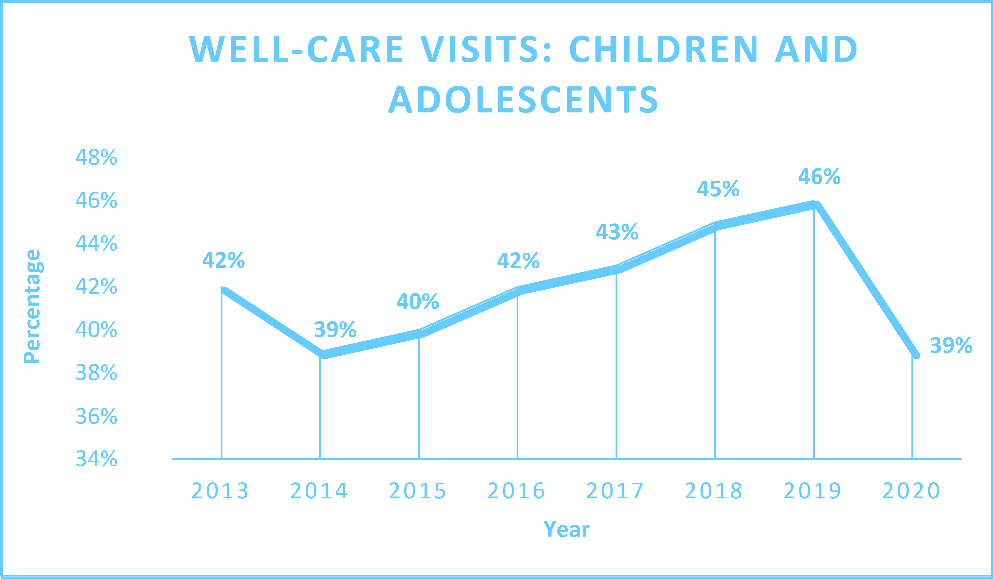
While there has been an overall positive trend in well-child visits and well-care visits, it is important to recognize that rates of visits remain low throughout the state. Notably in 2020, 40% of children 15 months and younger still do not receive the recommended six or more well-child visits with a primary care provider (PCP) after birth, and 35% of children 30 months and younger did not receive two visits with a PCP.
Breaking these metrics down by payer and region shows that more significant disparities exist.
Finding the Gaps: Pediatric Care by Region and Payer
One of the greatest variations in access to care for children exists between payers. When breaking out visits by children with commercial and Medicaid insurance, it is clear that children and adolescents with Medicaid do not receive the recommended number of visits as often as those with commercial insurance.
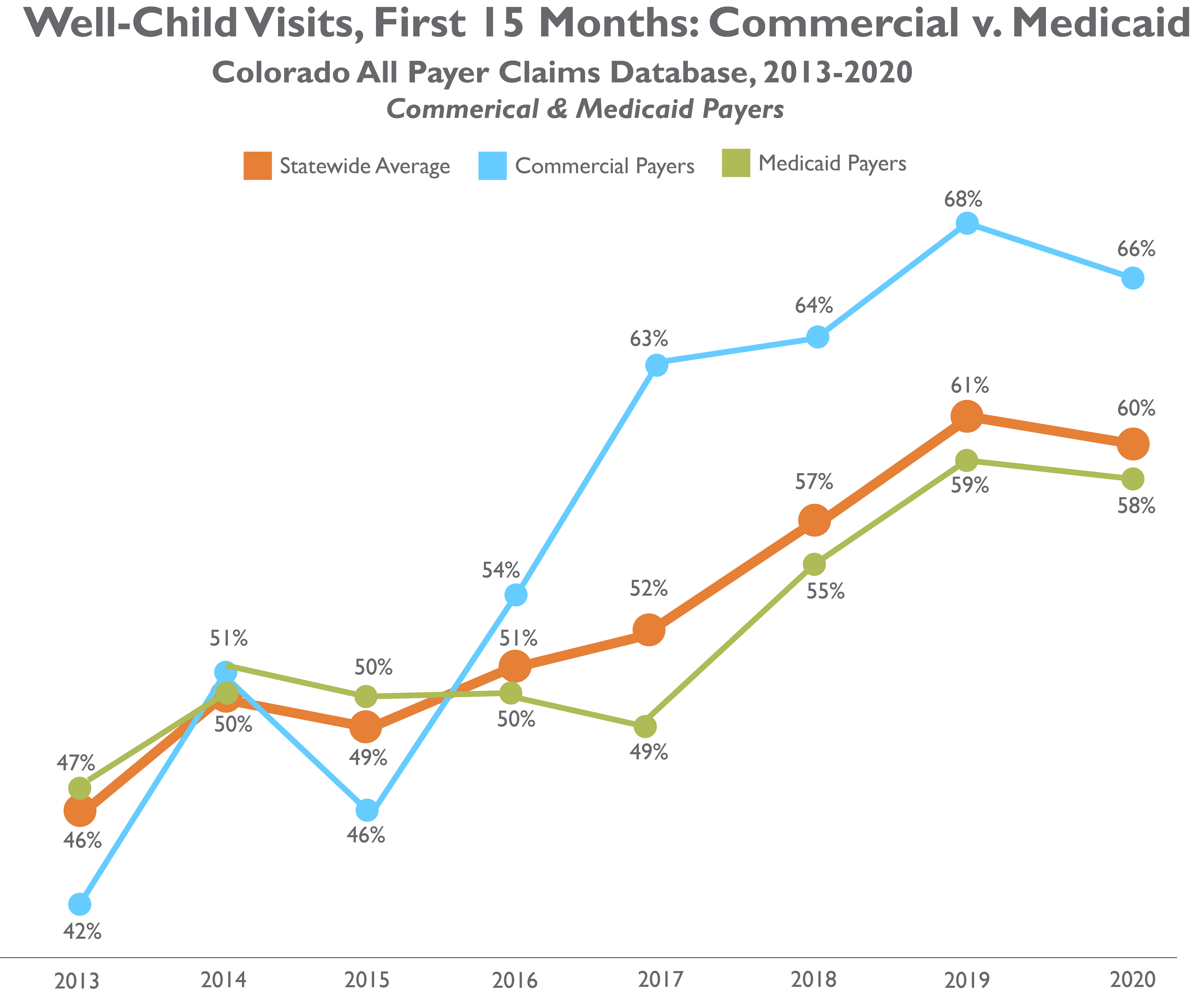
While visits for children covered by Medicaid are lower across all of the measures, it is especially noticeable for well-child visits for those 16-30 months and for children and adolescents. Visits for both age groups have consistently remained below the all payer statewide average, and significantly below rates for children with commercial insurance.
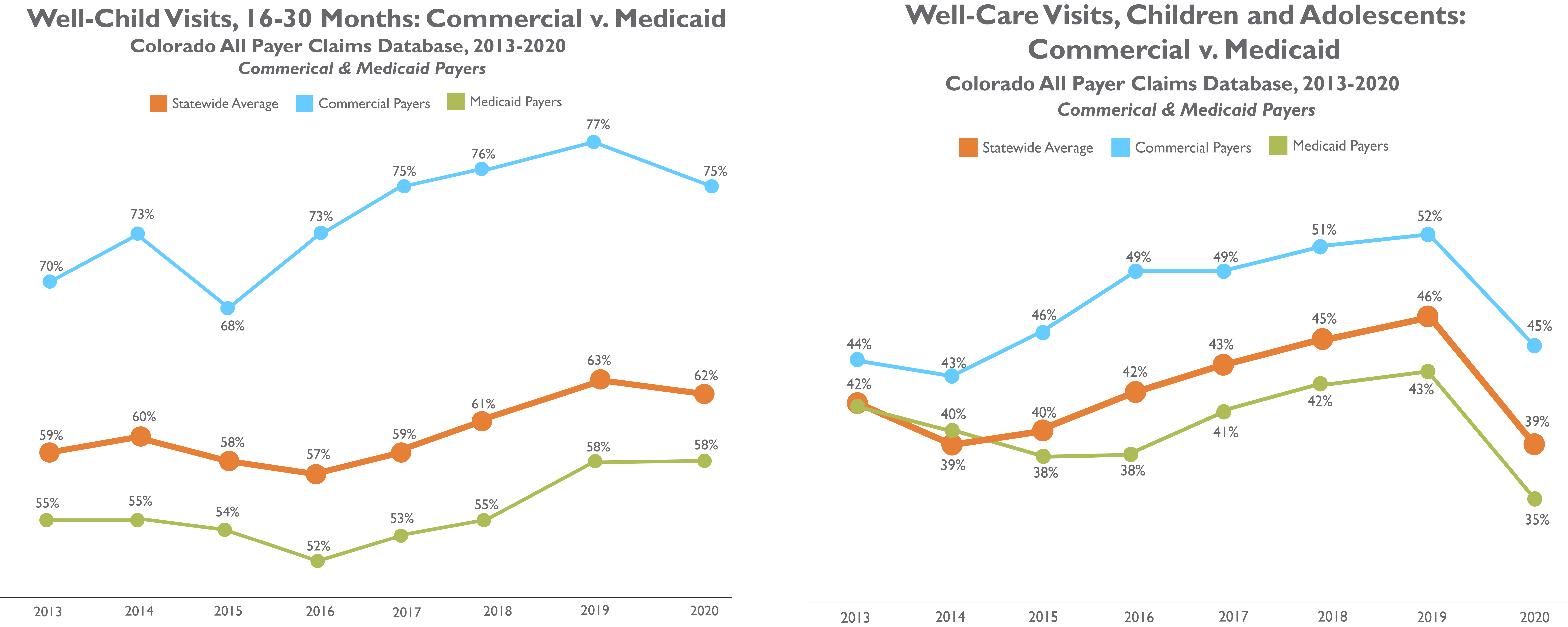
To continue improving pediatric care, the gap between insurance types should be addressed. However, considering regional groups in addition to payer breakouts adds an important layer that highlights the most disadvantaged groups.
Rural Care for Medicaid Patients
According to the data in the Community Dashboard, Medicaid patients in rural areas face the most significant barriers in accessing pediatric care. Numbers in both urban and rural regions 2013-2020 have tracked near a 40 percent increase.
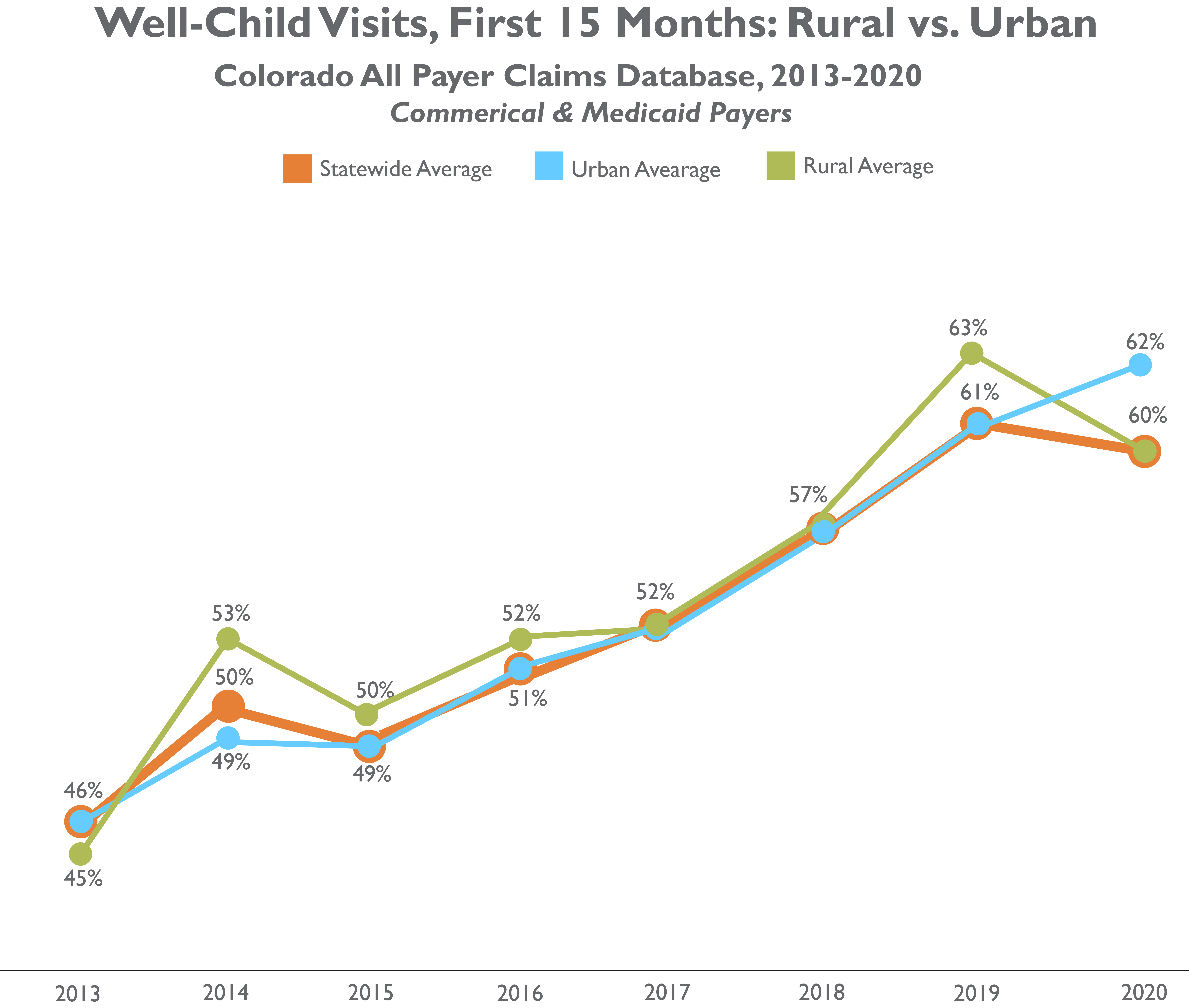
While there has been in an increase in access for both rural and urban patients, however, children with Medicaid have not seen similar gains. While visits for children up to 15 months with commercial coverage in rural areas increased by 77%, children with Medicaid receiving the recommended number of visits only increased by 30% from 2013 to 2020. In 2020, 71% of commercially covered children received six or more visits in the first three months of life compared to 60% of children in rural areas with Medicaid. In other words, 40% of children with Medicaid living in rural areas are not receiving their recommended visits.
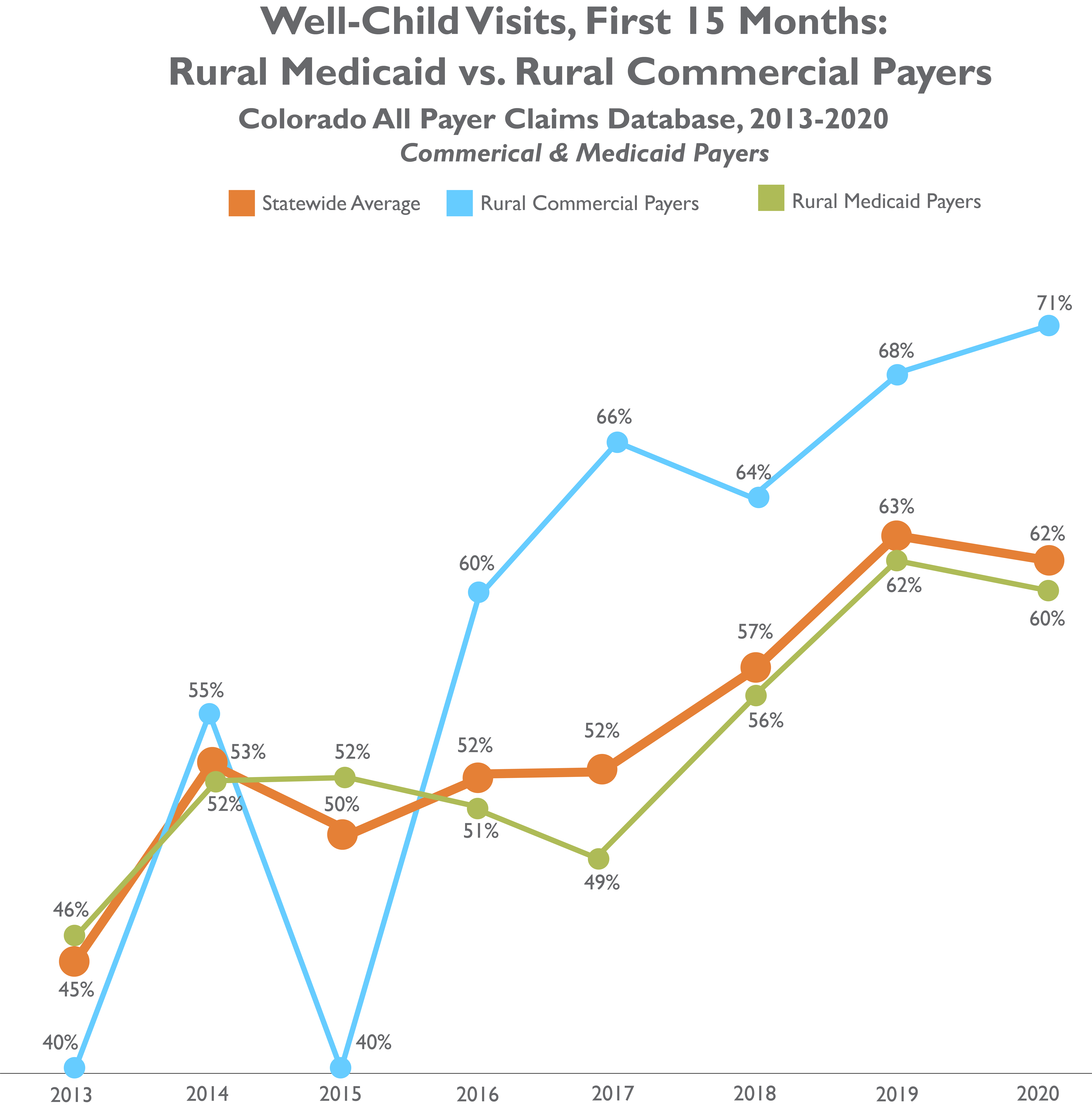
As with the breakouts by payer, the discrepancy for visits is most pronounced with older children. In 2020, 75% of children with commercial coverage aged 16-30 months received two visits with a PCP compared to 57% of children with Medicaid. And while numbers of children and adolescents receiving annual well-care visits in rural visits has remained low overall, never rising to even 50%, in 2020 – a year where patients receiving routine checks and care saw a sharp decline due to the COVID-19 pandemic – 42% of children with commercial insurance living in rural areas received an annual visit compared to just 31% among children with Medicaid.
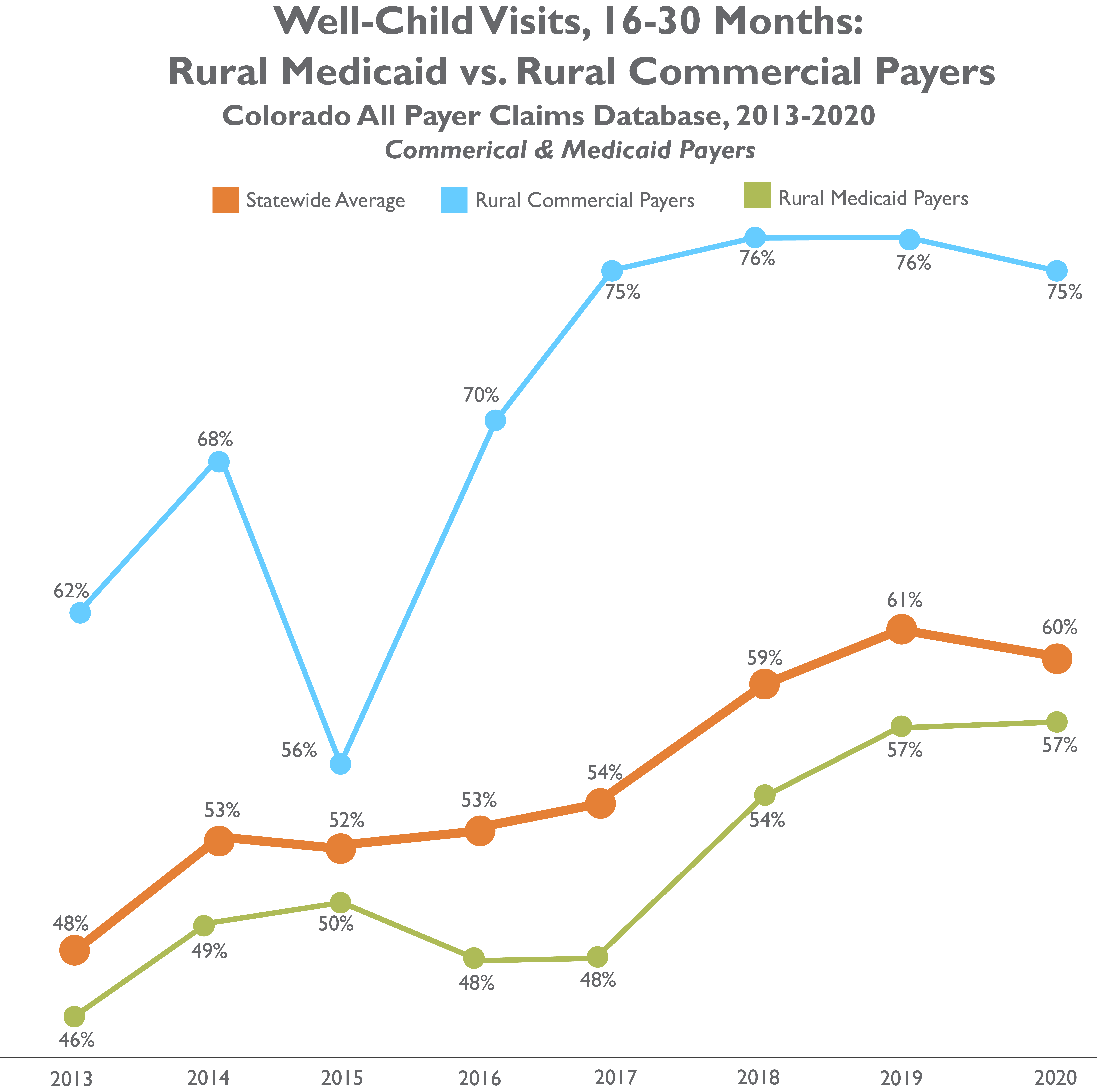
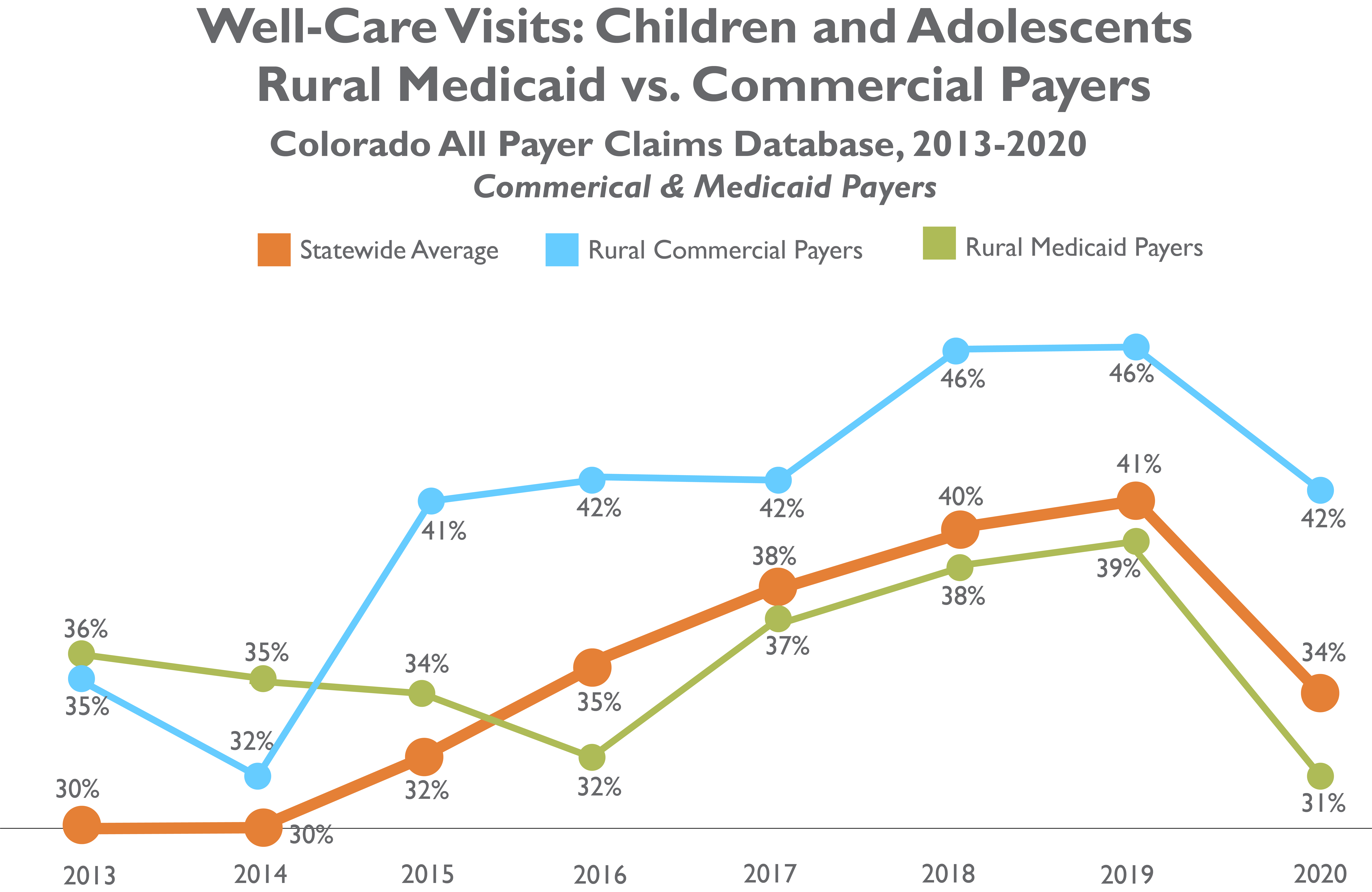
There are several possible reasons both well-child and child well-care visits are lower in rural areas and for children with Medicaid. Generally, people living in rural regions face more barriers to accessing care due to facility and provider shortages. It is time consuming to travel to an urban area to receive care, and it may not be feasible for some families. Coloradans with Medicaid who are living in rural regions also face health inequities that create bigger barriers to accessing care. Low income, lack of work time to take family to a doctor, language barriers, transportation issues, cultural concerns, and more can all impact the ability to access care, especially for parents and guardians whose children appear to be healthy and a well check doesn’t seem urgent or necessary.
By looking at data breakdowns on available in the Community Dashboard, Colorado communities and local health care systems can access how pediatric care varies in their area. With this knowledge, they can inform improvement initiatives to provide accessibility, raise awareness, and improve care at their local level.